Living with diabetes means managing more than just your blood sugar levels. Your oral health plays a surprisingly significant role in your overall diabetes management, and the connection between gum disease and diabetes works both ways. Research shows that people with diabetes are two to three times more likely to develop periodontal disease, and untreated gum disease can make blood sugar harder to control. Understanding this relationship is essential for protecting both your smile and your health.
At Advanced Periodontics of N.J., Dr. Gabriela Matei and Dr. Alexandru Peto specialize in helping patients navigate the complex relationship between periodontal health and systemic conditions like diabetes. With advanced education in periodontics and implant dentistry, our team provides comprehensive care that addresses both the oral and systemic aspects of gum disease.
How Diabetes Increases Your Risk for Gum Disease
Diabetes impairs your body’s ability to fight infection, making your gums more vulnerable to bacterial invasion. When blood sugar levels remain elevated, glucose builds up in your saliva, creating an ideal environment for harmful bacteria to thrive. These bacteria bind to food particles, forming plaque that irritates your gums and causes inflammation.
High blood sugar also reduces saliva production, causing dry mouth. Saliva normally helps clear away bacteria and neutralize acids in your mouth, so when you have less of it, your risk for both cavities and gum disease increases significantly. Diabetes can cause the salivary glands to make less saliva, and when less saliva is present, the likelihood of dental cavities and gum disease increases.
Additionally, diabetes weakens your white blood cells, which are your body’s primary defense against infections. This compromised immune response means that once gum disease develops, it progresses more rapidly and becomes more severe in people with diabetes compared to those without the condition.
How Gum Disease Affects Diabetes Management
The relationship between these two conditions doesn’t flow in just one direction. Gum disease can also affect insulin sensitivity and increase the risk of heart and kidney disease in diabetes patients. When you have periodontal disease, the chronic inflammation in your gums releases inflammatory markers into your bloodstream. These markers interfere with your body’s insulin function, making it harder for your cells to absorb glucose from your blood.
Periodontal infections create a constant state of inflammation in your body. Your immune system responds by releasing cytokines and other inflammatory mediators that promote insulin resistance. This creates a problematic cycle where poorly controlled diabetes worsens gum disease, and untreated gum disease makes blood sugar more difficult to manage.
The good news is that addressing gum disease can help improve glycemic control. Studies have shown that patients who receive periodontal treatment often see improvements in their A1C levels over time. This makes professional care an important component of comprehensive diabetes management.
Warning Signs You Shouldn’t Ignore
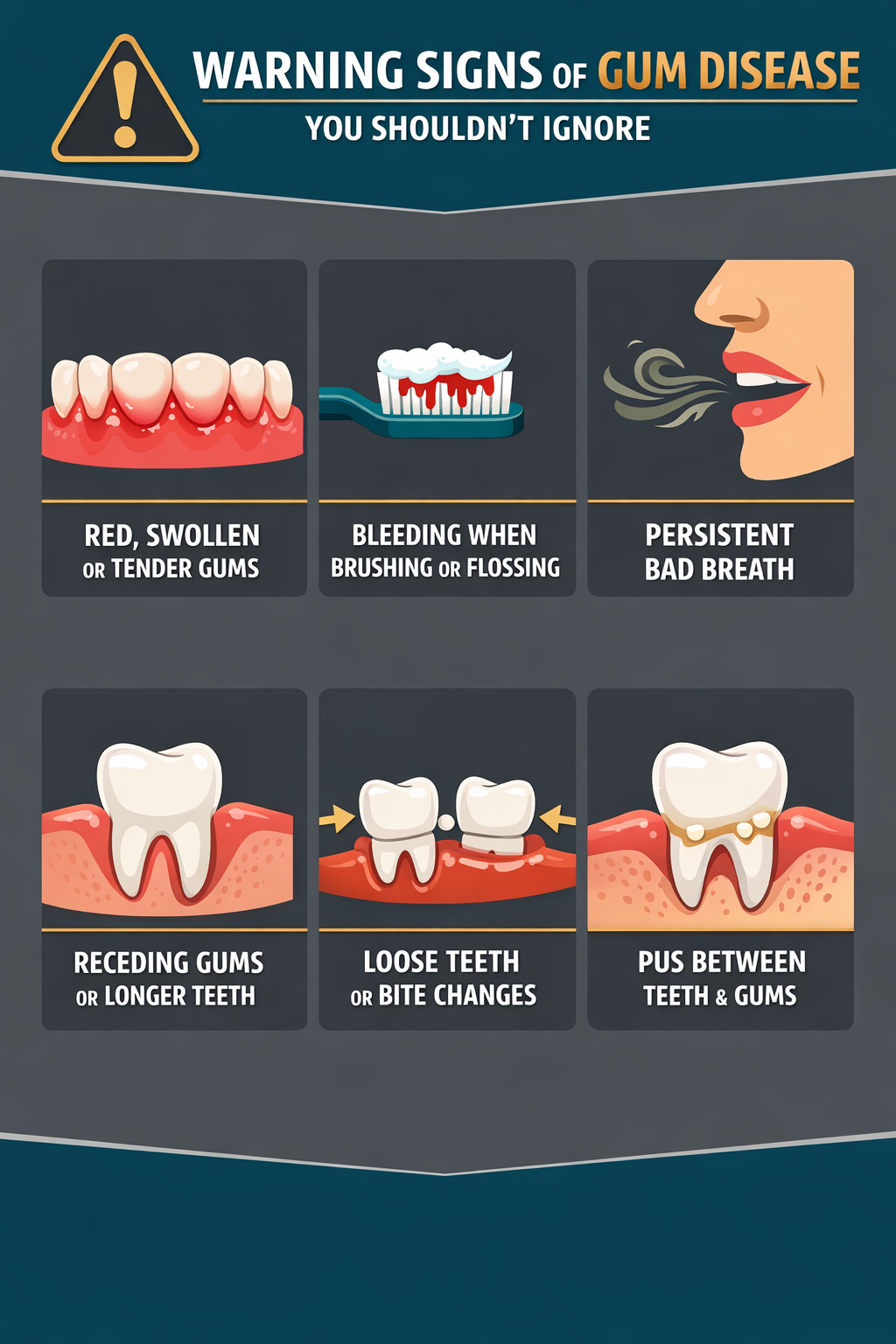
Pinpointing the early warning signs of gum disease is crucial for people with diabetes. You should schedule an appointment with a periodontist if you notice any of these symptoms:
- Red, swollen, or tender gums
- Bleeding when you brush or floss
- Bad breath or a lingering bad taste in your mouth
- Receding gums or teeth that appear longer
- Loose teeth or changes in your bite
- Pus between your teeth and gums
Early intervention can prevent these symptoms from progressing to advanced periodontal disease, which can lead to tooth loss and other serious complications.
Protecting Your Oral Health with Diabetes
Managing both conditions requires a proactive approach to your oral health. Brush your teeth at least twice daily with fluoride toothpaste, and floss once a day to extract plaque from between your teeth and under your gumline. These simple habits can substantially reduce your risk of developing gum disease.
Schedule regular dental checkups and professional cleanings every six months, or more often if advised by your periodontal specialist. During these visits, your dental team can detect early signs of gum disease and administer treatment before the condition worsens. Always inform your dental professionals that you have diabetes so they can tailor your care appropriately.
Maintaining good blood sugar control is equally important for protecting your gums. Work together with your diabetes care team to keep your A1C levels within your target range. When your blood sugar is well-managed, your body is better able to fight infections and heal from dental procedures. If you smoke, quitting is one of the most important steps you can take for both your diabetes and your oral health, as smoking significantly increases your risk for periodontal disease.
Take Control of Your Oral and Overall Health at Advanced Periodontics of N.J.
Understanding the connection between gum disease and diabetes empowers you to take control of both conditions. Dr. Matei is a LANAP-certified clinician who utilizes cutting-edge laser technology for minimally invasive periodontal treatments. Her research on biomaterials for tissue reconstruction and regeneration, along with her faculty experience at Columbia University and the University of Pennsylvania, ensures you receive evidence-based care that addresses the unique challenges of managing periodontal disease with diabetes.
Don’t wait until symptoms become severe. Contact our River Edge office today to schedule a comprehensive periodontal evaluation and discover how we can help you maintain optimal oral health while managing your diabetes.